Understanding the Pancreas and Pancreatic Cancer
%20-%20Edited.png)
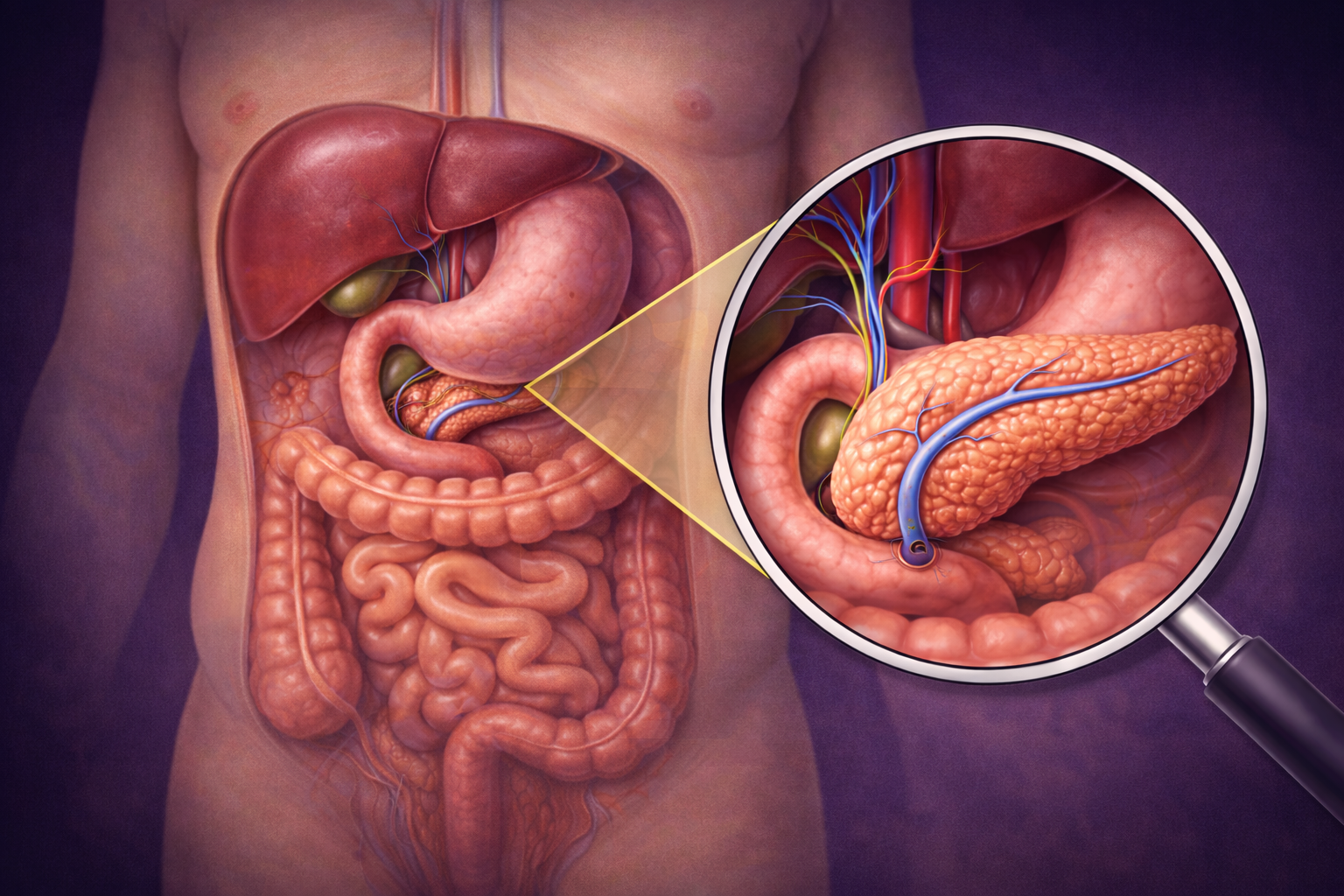
What is the Pancreas?
The pancreas is a vital organ in the digestive system, located deep in the abdomen behind the stomach. It is often referred to as the “hidden organ.” About six to eight inches long in adults, it has thin tubes that merge into a single duct opening into the intestine.
The pancreas produces digestive enzymes that break down fats, proteins, and carbohydrates for absorption. It also releases insulin into the blood, helping regulate sugar levels and maintain energy balance.
.jpg)
.gif)
What is Pancreatic Cancer?
Cancer is a disease where abnormal cells grow uncontrollably and can spread. Pancreatic cancer occurs when abnormal cells grow out of control in the tissue of the pancreas and form a tumour (an abnormal growth of tissue in any part of the body).
.jpg)
There is no effective screening test for pancreatic cancer, as a result pancreatic cancer is rarely diagnosed in the early stage.
This makes it important for individuals to pay attention to their bodies and be their own best advocate when they notice unusual symptoms.
Make an appointment with a healthcare professional to express your concerns.
.gif)
Types of Pancreatic Cancer
Not all pancreatic cancers are the same, and they shouldn’t be treated the same. A biopsy is needed to confirm a diagnosis.
Exocrine Tumors
(Approximately 92% of cases)
These start in the pancreas’s exocrine cells, which produce digestive enzymes. They are always cancerous and often aggressive. The most common type is adenocarcinoma.
Neuroendocrine Tumors (PNETs)
(Approximately than 8% of cases)
These grow in the hormone-producing cells of the pancreas. They can be cancerous or non-cancerous and usually grow more slowly than exocrine tumors.
Pancreatic Cancer Diagnosis
Pancreatic cancer is hard to detect and often isn’t diagnosed until it has grown significantly. Only approximately 20% of cases are caught early, while 40-50% are found after the cancer has spread.
If symptoms appear, doctors may order several tests to help diagnose the disease. Thes tests may be requested based on symptoms and accessibility.

The Reality in Canada
In 2026, pancreatic cancer will affect 7,100 Canadians.
Men impacted
Women impacted
New cases every day
Signs and Symptoms of Pancreatic Cancer
Pancreatic cancer symptoms are often mild, vague, or come and go, varying from person to person. They are often mistaken or misdiagnosed for other diseases such as: pancreatitis (inflammation of the pancreas), gallstones, irritable bowel syndrome (IBS) or hepatitis (inflammation of the liver).
Since the pancreas is deep in the abdomen, doctors cannot feel tumors during a physical exam. These factors make early detection challenging, which is why imaging and other diagnostic tests are essential.

Signs & symptoms
If you are experiencing changes in your body, and they involve 1 or more of these symptoms, please seek medical attention and take this information with you, to reference pancreatic cancer.
Additional Signs and Symptoms can include:
• Blood Clots (Deep Vein Thrombosis)
• Fatigue
Pain may occur in the upper abdomen or middle of the back and can come and go. It may worsen when lying down or after eating, and is often caused by the tumour pressing on nearby nerves or organs.
Jaundice occurs when bile builds up in the body due to a blockage in the bile duct. This may cause yellowing of the skin or eyes, dark urine, pale stools, and itching.
Urine may appear darker than usual when bilirubin levels increase in the blood. This can happen even before jaundice is noticeable.
Stools may become pale, greasy, or float. This can occur when digestive enzymes from the pancreas are reduced, affecting how fats are broken down.
In some cases, pancreatic cancer can affect insulin production, leading to a sudden diagnosis of diabetes, particularly in adults over 50 with no prior history.
Symptoms can include indigestion, nausea, bloating, gas, or a loss of appetite. These issues are often mistaken for common gastrointestinal conditions.
New or worsening feelings of depression, anxiety, or emotional distress can sometimes appear early and may be linked to chemical changes in the body.
New or worsening feelings of depression, anxiety, or emotional distress can sometimes appear early and may be linked to chemical changes in the body.
Pancreatic Cancer Risk Factors
The exact cause of pancreatic cancer is often unknown, but certain risk factors may increase a person's chances of developing pancreatic cancer. Some risk factors for pancreatic cancer can be controlled, while others cannot be.
Understanding these risks can help with prevention and early detection.
While we can’t control genetics or age, lifestyle choices like quitting smoking, eating well, and maintaining a healthy weight can help lower the risk.
Smokers are twice as likely to develop pancreatic cancer. Quitting smoking reduces this risk.
Smokers are twice as likely to develop pancreatic cancer. Quitting smoking reduces this risk.
Smokers are twice as likely to develop pancreatic cancer. Quitting smoking reduces this risk.
Smokers are twice as likely to develop pancreatic cancer. Quitting smoking reduces this risk.
People who consume high amounts of alcohol have an increased risk of developing pancreatic cancer. Reducing or avoiding alcohol can help lower this risk.
Long-term contact with gasoline, insecticides, and industrial chemicals may be linked to pancreatic cancer. Avoiding prolonged exposure could help.
Inherited conditions like BRCA mutations, Lynch syndrome, Peutz-Jeghers syndrome, and hereditary pancreatitis increase risk. Those with a family history should talk to a doctor about genetic screening.
Most cases occur in people over 60.
Often caused by heavy alcohol use or smoking. Reducing these habits may lower the risk.
Higher rates are seen in African Canadians and Ashkenazi Jews.
Cirrhosis, chronic pancreatitis, and past digestive surgeries may increase risk.
People with long-standing diabetes have a higher risk of developing pancreatic cancer. Managing blood sugar levels may help reduce this risk.
Long-term exposure to certain chemicals and heavy metals may increase the risk of pancreatic cancer. Limiting or avoiding prolonged exposure can help reduce this risk.
Chronic gum disease has been linked to an increased risk of pancreatic cancer. Maintaining good oral hygiene and regular dental care may help reduce this risk.
Diagnostic Tests
An overview of the tests used to help detect and diagnose pancreatic cancer.

Blood Tests
No single blood test can confirm pancreatic cancer. However, doctors may check:
• CBC (Complete Blood Count)
• Bilirubin
• Liver function tests (LFTs)
• INR (clotting test)
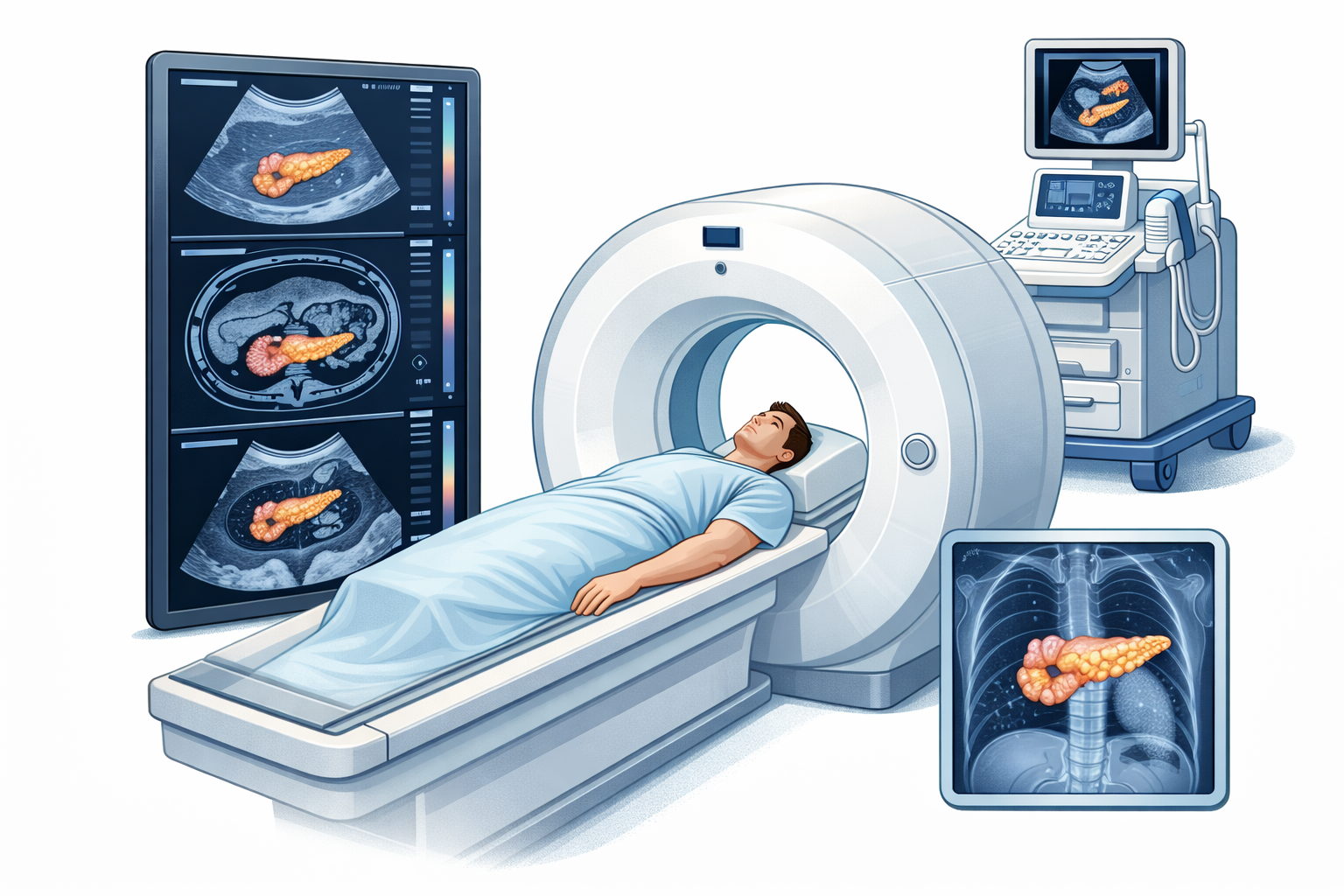
Imaging Tests
• Ultrasound – Helps rule out other causes like gallstones. It’s quick, safe, and doesn’t use radiation.
• CT Scan (Pancreatic Protocol) – Uses contrast dye to create detailed images. This test can detect 98% of pancreatic cancers and metastases. Side effects may include a warm sensation or metallic taste.
• MRI (Magnetic Resonance Imaging) - A painless scan that provides clear images of soft tissues. It does not require drinking contrast or injections. Commonly used for brain, nerve, and muscle imaging but can help detect pancreatic tumors.
• PET Scan (Positron Emission Tomography) - Often combined with CT or MRI scans for more precise results. Provides both anatomical (structure) and metabolic (function) information. Helps locate cancerous areas more accurately.

Serum Tumor Markers
Certain markers in the blood may suggest pancreatic cancer but are not used for diagnosis alone:
• CA19-9
• CEA
• LFTs & Bilirubin
• Glucose level changes
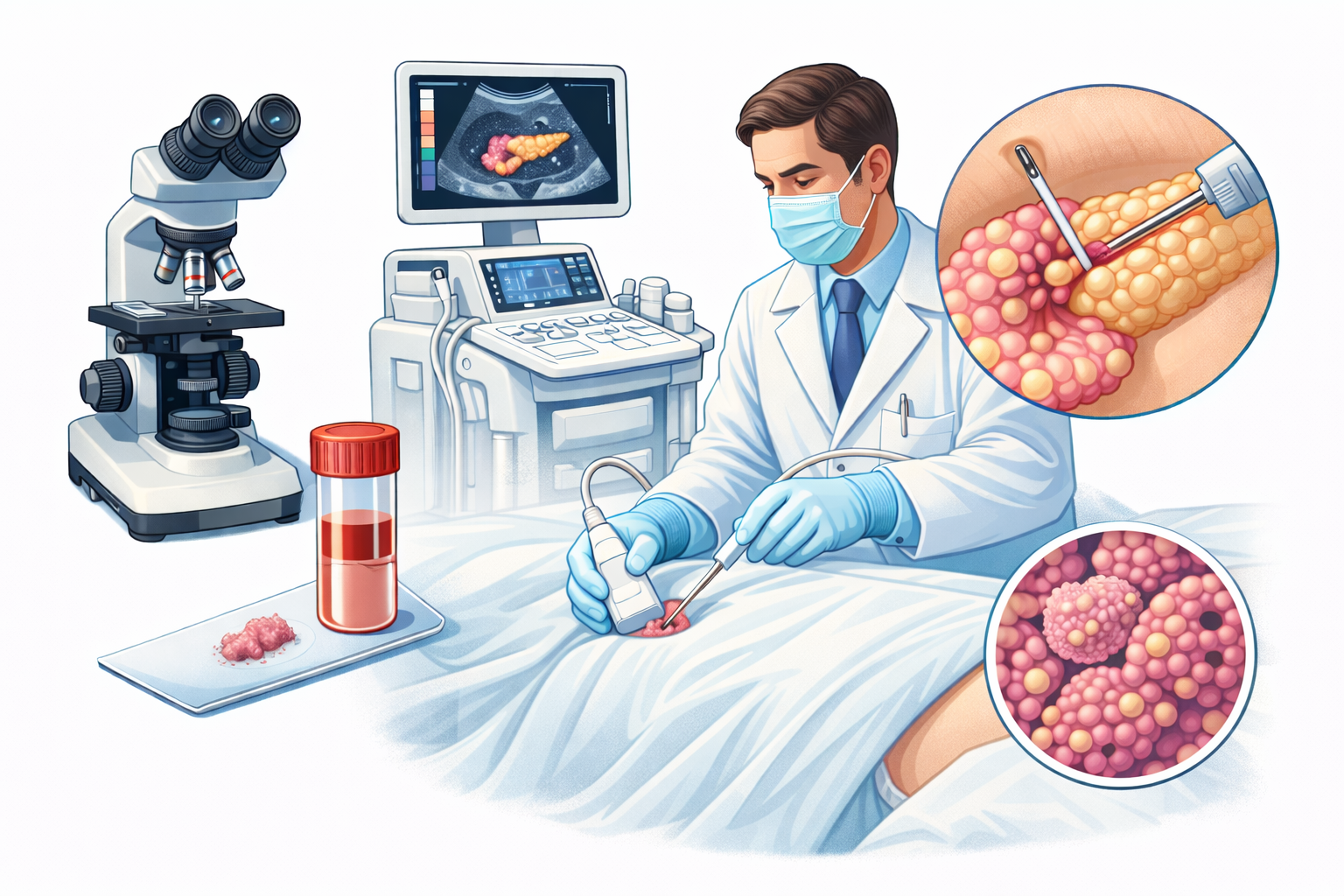
Biopsy – The Only Way to Confirm Cancer
A biopsy is necessary to not only diagnose pancreatic cancer but the type of tumour you have. A tissue sample is examined under a microscope to confirm the type of cancer.
About 10% of pancreatic cancers are neuroendocrine tumors, which have a better prognosis. Other rare cancers, like lymphomas or metastases from other organs, can also affect the pancreas.
If a suspicious mass is found, a biopsy should be done as soon as possible to determine the best treatment. Clinical trials should be investigated upon a diagnosis and biopsy.
ERCP (Endoscopic Retrograde Cholangiopancreatography) - This procedure uses a dye to check for blockages in the bile and pancreatic ducts. A thin tube is passed down the throat into the small intestine. Doctors can collect tissue samples for testing.
Additionally, it is useful for jaundice patients – A stent can be placed to keep ducts open, relieving symptoms.
Diagnostic Tests
An overview of the tests used to help detect and diagnose pancreatic cancer.
Blood Tests
No single blood test can confirm pancreatic cancer. However, doctors may check:
• CBC (Complete Blood Count)
• Bilirubin
• Liver function tests (LFTs)
• INR (clotting test)
Imaging Tests
• Ultrasound – Helps rule out other causes like gallstones. It’s quick, safe, and doesn’t use radiation.
• CT Scan (Pancreatic Protocol) – Uses contrast dye to create detailed images. This test can detect 98% of pancreatic cancers and metastases. Side effects may include a warm sensation or metallic taste.
• MRI (Magnetic Resonance Imaging) - A painless scan that provides clear images of soft tissues. It does not require drinking contrast or injections. Commonly used for brain, nerve, and muscle imaging but can help detect pancreatic tumors.
• PET Scan (Positron Emission Tomography) - Often combined with CT or MRI scans for more precise results. Provides both anatomical (structure) and metabolic (function) information. Helps locate cancerous areas more accurately.
Serum Tumor Markers
Certain markers in the blood may suggest pancreatic cancer but are not used for diagnosis alone:
• CA19-9
• CEA
• LFTs & Bilirubin
• Glucose level changes
Biopsy – The Only Way to Confirm Cancer
A biopsy is necessary to not only diagnose pancreatic cancer but the type of tumour you have. A tissue sample is examined under a microscope to confirm the type of cancer.
About 10% of pancreatic cancers are neuroendocrine tumors, which have a better prognosis. Other rare cancers, like lymphomas or metastases from other organs, can also affect the pancreas.
If a suspicious mass is found, a biopsy should be done as soon as possible to determine the best treatment. Clinical trials should be investigated upon a diagnosis and biopsy.
ERCP (Endoscopic Retrograde Cholangiopancreatography) - This procedure uses a dye to check for blockages in the bile and pancreatic ducts. A thin tube is passed down the throat into the small intestine. Doctors can collect tissue samples for testing.
Additionally, it is useful for jaundice patients – A stent can be placed to keep ducts open, relieving symptoms.





.avif)