Managing Pancreatic Cancer Pain
%20-%20Edited.png)
FACT: Effective pain management is crucial for quality of life in people with pancreatic cancer. Each individual experiences pain differently, influenced by both physical and psychological factors.
Pain from pancreatic cancer can be treated successfully. Working closely with your healthcare team and asking for a referral to a pain management specialist is strongly recommended. Good pain control improves quality of life, helps you focus on daily activities, and reduces stress for both patients and families.

What Causes Pain in Pancreatic Cancer?
Pain can come from several sources:
- Tumor growth – Rapid tumor expansion can cause:
- Swelling and inflammation
- Blockage of bile, pancreatic enzymes, or bowel contents
- Pressure on or invasion of nearby nerves or organs
- Treatment side effects – Chemotherapy, radiation, or surgery may cause pain
- Common pain locations – Mid-abdomen often radiating to the back
If untreated, pain can lead to anxiety, depression, and decreased quality of life.
Early Steps: Track and Talk About Your Pain
- Speak with your doctor as soon as you notice pain – don’t wait until it’s severe
- Keep a pain journal:
- Location of pain
- Type (sharp, dull, throbbing, burning)
- Strength (1–10 scale)
- Frequency and duration
- Triggers (e.g., eating)
- What helps or worsens the pain
This helps your healthcare team develop the best pain management plan for you.
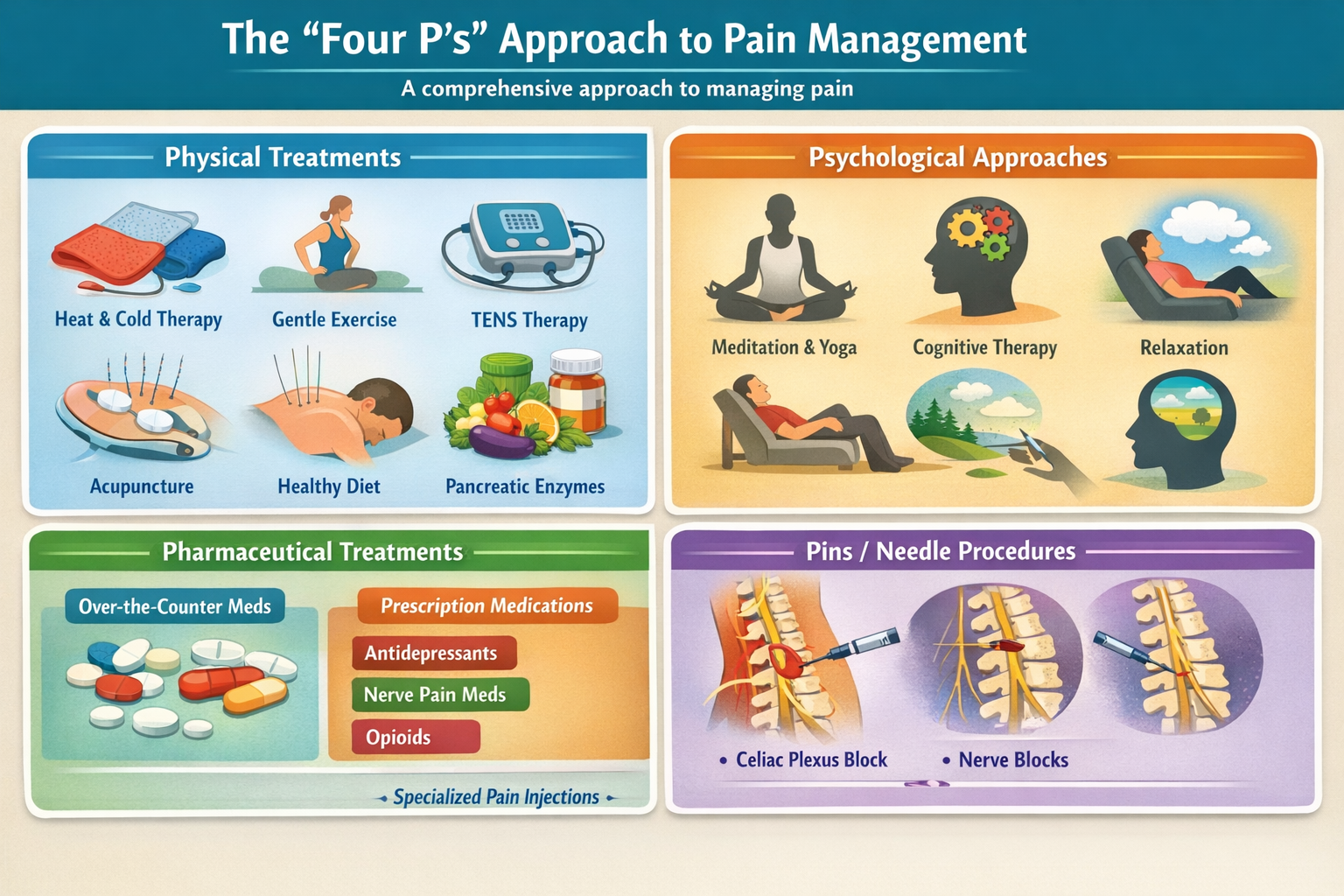
The “Four P’s” Approach to Pain Management
Effective pain management looks at the whole person using four approaches:
1. Physical Treatments
- Heat or cold compresses
- Rest and gentle movement
- TENS (electrical nerve stimulation)
- Acupuncture
- Diet adjustments
- Pancreatic enzymes (can reduce pain after eating)
2. Psychological Approaches
- Meditation, mindfulness, Qi Gong, or yoga
- Cognitive Behavioural Therapy (CBT)
- Relaxation and visualization exercises
3. Pharmaceutical Treatments
Mild pain (over-the-counter):
- Tylenol® (acetaminophen)
- Advil®, Motrin® (ibuprofen)
- Aleve® (naproxen)
- Topical diclofenac (Voltaren)
Moderate pain (first-line prescriptions, may take 3–6 weeks):
- Tricyclic antidepressants: Amitriptyline (Elavil), Nortriptyline (Aventyl)
- Gabapentin family: Gabapentin (Neurontin), Pregabalin (Lyrica)
- New antidepressants: Duloxetine, Venlafaxine
- “Almost opioids”: Tramadol, Tramacet, Tapentadol (Nucynta)
Moderate to strong pain (opioids):
- Weak: Codeine (Tylenol #3)
- Strong: Morphine, Oxycodone, Hydromorphone, Methadone
- Side effects: constipation, drowsiness (usually manageable with your doctor)
Other options:
- Cannabinoids: THC, CBD
- Prescription sprays: Sativex (THC:CBD 50:50), Nabilone (synthetic THC)
Steroids for swelling/pressure-related pain:
- Prednisone (Deltasone®), Dexamethasone (Decadron®)
Anti-seizure meds for nerve pain:
- Gabapentin (Neurontin®), Phenytoin (Dilantin®)
4. Pins / Needle Procedures
- Coeliac Plexus Block:
- Injection to block abdominal and back pain
- Performed by a pain specialist or radiologist
- Relief lasts ~6 months and can be repeated
- Works for ~80% of patients
- Rare but serious risk: accidental spinal injection
Additional Pain Management Options
- Stent Placement: Relieves blockages in the bile duct or bowel to ease pain, vomiting, or jaundice
- Radiation and Steroids: Reduce tumor size, swelling, and inflammation
- Palliative Surgery: Part of the tumor removed or bowel bypassed to improve comfort
Non-Drug Approaches
- Acupuncture, massage, hypnosis
- Physical or occupational therapy
- Hot or cold compresses
- Meditation, relaxation exercises
Final Notes: Advocating for Your Pain Management
- You deserve the best pain control options available
- Don’t wait for severe pain – it’s easier to manage when mild
- Follow your medication schedule carefully
- Speak openly with your healthcare team about your pain
- Ask for a pain management specialist early
- Remember: Pain from pancreatic cancer can be controlled. Effective management improves both your quality of life and the lives of your loved ones.


.avif)